Your Guide to Surviving a Dermatology Modifier 25 Audit

A dermatology modifier 25 audit requires you to prove one thing: that the Evaluation and Management (E/M) service you billed, such as for a new patient visit (CPT 99203), was "significant and separately identifiable" from a procedure, like a biopsy (CPT 11102), performed on the same day. Per CMS and AAPC guidelines, if your documentation does not create a clear, distinct narrative for both the cognitive E/M work and the procedure, payers will deny the claim and may launch a full audit. With dermatology practices squarely in the audit spotlight, mastering this documentation is critical for practice managers and physician owners to protect revenue.
Why Payers Are Cranking Up Dermatology Modifier 25 Audits

If it feels like your modifier 25 claims are getting more side-eye from payers, you’re not imagining things. Dermatology practices have become a prime target, and the reason is simple: the sheer volume of claims that pair an E/M service with a minor procedure.
From an auditor’s point of view, seeing CPT code 99213 (an established patient E/M) billed with modifier 25 alongside a procedure like 17110 (destruction of benign lesions) over and over again is a huge red flag. They immediately start to question whether the E/M was actually necessary or if it was just routine care that should have been bundled into the procedure’s payment.
The CMS Definition Is Your Only Defense
Your entire argument in a modifier 25 audit rests on the official CMS definition. The E/M service must be "significant and separately identifiable." This isn't just a guideline; it's the yardstick your documentation will be measured against.
The question every auditor is trained to ask is this: "Does the note clearly show the thinking and decision-making for a problem that stands apart from the procedure itself?" If your chart note reads like one continuous story, you will lose the audit.
This means your documentation has to tell two different stories. One story is the evaluation and management of a specific patient complaint. The second story is about performing the procedure. Without that clean break, payers will just assume the E/M work was incidental.
The Financial Stakes and a Scathing OIG Report
Failing a modifier 25 audit isn't just about losing payment on one claim. Payers use a method called extrapolation, where they turn a few failed claims from a small sample into a massive refund demand that can cripple your revenue.
This isn't a hypothetical threat. The U.S. Department of Health and Human Services Office of Inspector General (OIG) proved it. They launched a targeted review after discovering that in 2019, a staggering 56% of dermatologists' Medicare claims with an E/M service also included a minor procedure on the same day.
While their review found that dermatologists got it right on 90 out of 100 claims, those 10 failed claims were extrapolated to a nationwide overpayment of $62,915,655. That level of federal scrutiny puts every single dermatology practice on notice. For practice managers and physicians, mastering the rules of dermatology billing isn't just good practice anymore—it's a survival tactic.
Building Your Proactive Audit Defense Playbook
The best defense against a payer audit isn't hoping it won't happen. It's building a strong offense—a proactive internal auditing program designed to find and fix your modifier 25 weak spots before they become a seven-figure clawback.
A solid playbook means moving from reacting to auditor demands to building a resilient practice. It involves a repeatable workflow: selecting the right claims to review, scoring them against a clear rubric, and fixing the root cause of any errors you find.
This is the typical path that leads to a full-blown audit. It almost always starts with high utilization numbers that catch a payer's eye.
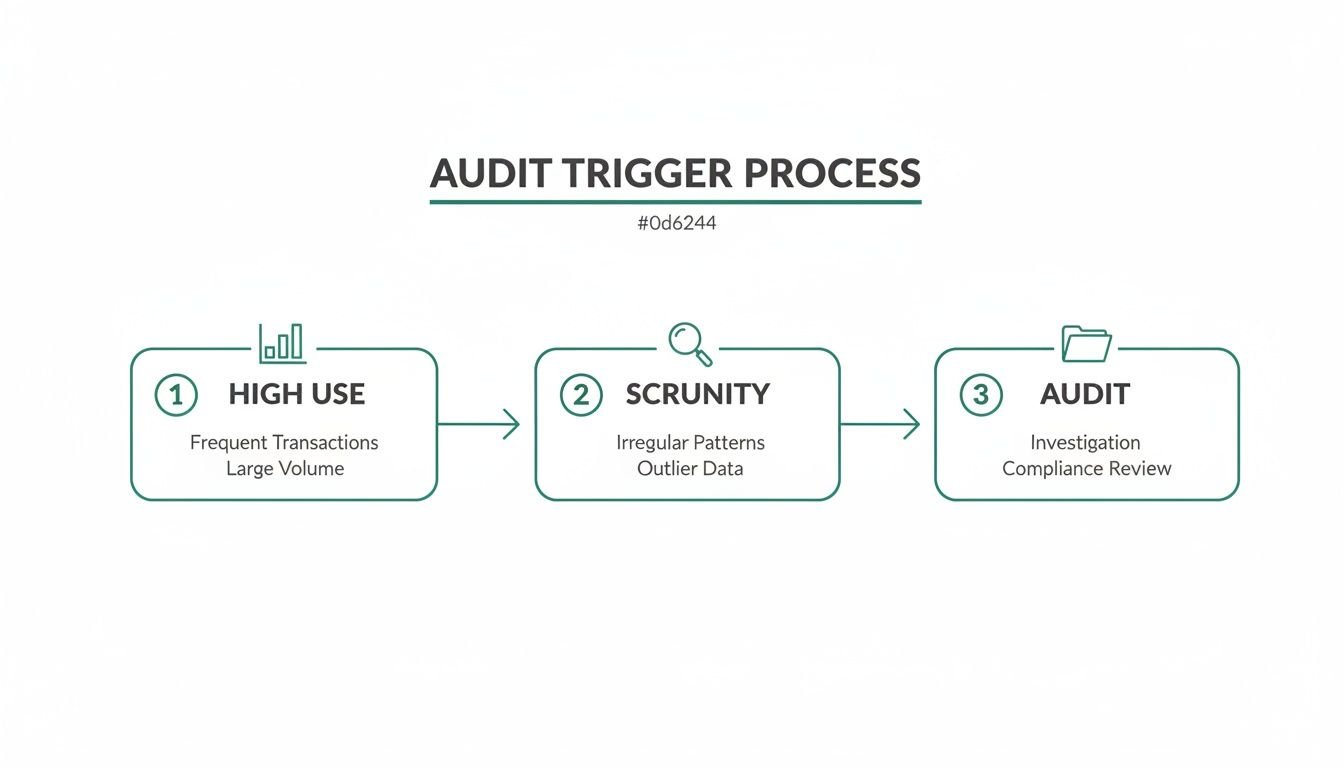
As you can see, consistent high usage of specific code pairs is what gets you on the radar. That initial scrutiny often escalates into a formal records request and a painful audit process.
Selecting Your Audit Sample
Waiting for denials to tell you there's a problem is a failing strategy. You need to stress-test your own claims before a payer does it for you. The trick is to create a sample that's big enough to be statistically relevant but small enough to be manageable for your team.
A great place to start is auditing 15 charts per provider, per quarter. This gives you enough data to spot dangerous trends without getting bogged down.
You’ll want to focus these audits on the code combinations that are under the most intense scrutiny. For nearly every dermatology practice, this means looking closely at:
- 99213-25 with 17110: An established patient visit paired with the destruction of benign lesions.
- 99214-25 with 17000: An established patient visit with the destruction of premalignant lesions.
- 99203-25 with 11102: A new patient visit combined with a tangential skin biopsy.
These pairs are perpetually on payer watchlists. By reviewing them yourself, you get to see exactly what an external auditor will see first. You can build out this foundation by referencing our complete revenue cycle management checklist to make sure all your bases are covered.
Designing an Audit Scoring Rubric
Once you’ve pulled your sample, you need an objective way to grade the documentation. Don't rely on gut feelings. Your scoring rubric should be built directly from CMS guidelines and AAPC standards to take all the subjectivity out of the review.
Your rubric needs to answer three critical questions for each chart:
- Is the Chief Complaint Clear? Does it plainly state a problem that requires a separate E/M service, one that stands apart from the scheduled procedure?
- Is the HPI Distinct? Is the History of Present Illness (HPI) for the E/M problem completely separate from the discussion about the procedure itself?
- Are the Exam and Procedure Notes Separate? Can an auditor easily draw a line where the physical exam for the E/M service ends and the pre-operative work for the procedure begins?
A simple "pass/fail" system for each of these three points creates a clear, actionable score. If a chart fails on any one of them, it’s a red flag—it would likely fail a real-world audit.
This structured approach delivers hard data. It helps you pinpoint specific weaknesses, whether it's a single provider's documentation habits or a faulty EHR template causing problems across the entire practice.
When it comes to a modifier 25 audit, your EHR documentation isn't just a record of patient care—it's the only evidence you have. An auditor's job is to find reasons to deny payment. If your note doesn't tell a crystal-clear story of two distinct services, you've already handed them the win.
The entire defense rests on structuring the note so the history, exam, and medical decision-making for the E/M service are completely walled off from the procedural part. Let's walk through exactly how this plays out in a busy dermatology clinic.
A Tale of Two Services in One Visit
Imagine a patient, Sarah, is on the schedule for a follow-up to treat several actinic keratoses (AKs) on her forearms with cryotherapy. That planned procedure is CPT 17000 (Destruction, premalignant lesions; first lesion).
But during the visit, she points to a mole on her back. "This spot has been changing color and getting bigger," she says. "It's been worrying me for a few months."
That new complaint is your trigger. It kicks off a significant, separately identifiable E/M service. The work you do to evaluate that changing mole is entirely separate from the planned cryotherapy. Your documentation must make this separation obvious, or an auditor will bundle the services and claw back the E/M payment.
To dig deeper into the official rules, you can review our complete guide on the proper use of CPT modifier 25.
Documenting a Claim That Can't Be Denied
The way you write the note is everything. An auditor should be able to draw a line in your documentation where the E/M service ends and the procedure begins. This is where EHR smart phrases and templates can become a double-edged sword; they save time but often create generic "note bloat" that blurs the lines between the two services.
Let’s look at a non-compliant note side-by-side with one that’s built to withstand an audit.
Modifier 25 Documentation Examples
This table contrasts a high-risk note with a low-risk, compliant one for our common scenario. Notice how the compliant version creates two distinct "mini-notes" within the same encounter.
| Scenario Element | Non-Compliant Documentation (High Audit Risk) | Compliant Documentation (Low Audit Risk) |
|---|---|---|
| Chief Complaint | "Follow-up for AKs. Patient has other concerns." | "1. F/U actinic keratosis for cryo. 2. New, changing nevus on back." |
| HPI | "Patient here for cryo of AKs on forearms. Also notes changing mole on back. No other complaints." | "HPI (Nevus): Patient notes a 6mm nevus on her mid-back has become darker and grown over the past 3 months. Reports occasional itching. No bleeding or pain." |
| Exam | "Exam of skin shows multiple AKs on forearms. Mole on back is dark and irregular. Proceeding with cryo." | "Exam (Nevus): On the mid-back, there is a 6mm dark brown macule with irregular borders and color variegation. The rest of the skin exam is deferred. Exam (Procedure): Multiple 2-4mm hyperkeratotic papules on bilateral forearms consistent with AKs." |
| Assessment/Plan | "1. Actinic Keratosis – Cryotherapy. 2. Atypical Nevus – Monitor." | "A/P (E/M Service): 1. Atypical Nevus (D49.2): High suspicion for melanoma. Discussed risks/benefits of biopsy. Patient agrees to proceed with shave biopsy today. A/P (Procedure): 2. Actinic Keratosis (L57.0): Performed cryotherapy x5 lesions on forearms." |
The difference is stark. The compliant note dedicates specific sections to the history and exam for the new problem (the nevus), which justifies the E/M. It physically separates that assessment and plan from the one for the planned procedure.
The single biggest failure in non-compliant notes is commingling. When the exam and assessment for the E/M problem and the procedure are blended into a single narrative, an auditor will conclude the E/M was incidental and not separately billable.
Avoiding the Most Common Documentation Traps
Even well-meaning providers fall into documentation habits that are like waving a red flag at an auditor. These are the traps we see most often:
- Cloned Notes: Copying and pasting from a previous encounter without significant, relevant updates is a gift to auditors. They run software to detect notes that are too similar, suggesting the E/M service wasn't truly unique to that day's visit.
- Generic Templates: A single, all-purpose template for visits that include a procedure almost guarantees a blended, non-compliant narrative. It forces the documentation into a format that hides the separate work.
- Vague Details: Simply writing "Patient has other concerns" is worthless. You have to document the history, review of systems, and exam directly related to those other concerns to prove you performed separate cognitive work.
The fix is often simple. Create separate "smart phrases" or mini-templates specifically for common E/M drivers, like a "New Lesion Evaluation" block. This lets your team quickly insert a structured, compliant chunk of text, ensuring the cognitive work is clearly documented and segregated from the procedure—every single time.
Navigating Payer-Specific Rules and Denials
Successfully billing modifier 25 isn’t about following one set of rules; it’s about mastering many. Each payer—from your local Medicare contractor to giants like Cigna and UnitedHealthcare—has its own distinct, and often conflicting, policies. This creates a minefield of audit traps for dermatology practices that take a one-size-fits-all approach to billing.
The real challenge is that while CMS provides the foundational definition of modifier 25, commercial payers are free to add their own layers of requirements. A claim that sails through your MAC might get an instant denial from a commercial plan for the exact same service, just because their internal payment policy is stricter. That variability is precisely why a proactive defense is essential.
Decoding Common Denial Reasons
When a modifier 25 claim gets denied, the reason code might feel vague, but it’s sending a specific message. Understanding these codes is the first step in building a powerful appeal. Most denials fall into a few key buckets.
- Service Incidental to Procedure: The payer decided the E/M work was just routine pre- or post-op care that’s already bundled into the procedure’s payment.
- Bundling: The payer’s automated system flagged the E/M and procedure codes as a pair that shouldn't be billed together.
- Lack of Medical Necessity for E/M: An auditor reviewed the note and concluded there was no legitimate medical reason for the E/M service itself.
Notice a pattern? These denials all point back to a single root cause: your documentation failed to prove the E/M service was significant and separately identifiable.
The burden of proof is always on the practice. A denial for "bundling" is just the payer’s way of saying, "You didn't convince us this work was separate." Simply resubmitting the claim without new evidence is a wasted effort.
For example, a denial on a 99213-25 with a 17110 (destruction of benign lesions) almost always means the note didn't clearly separate the evaluation of a new, unrelated problem from the work of performing the destruction.
Payer Policies Signal Future Audit Trends
Payers often broadcast their audit intentions through policy updates, and it pays to listen. Cigna, for one, has been particularly aggressive in its scrutiny of modifier 25. This focus is a direct response to soaring denial rates in dermatology, which can hit between 32% and 48%—a number that dwarfs the general industry average of 8-12%.
Dermatology practices face this heat primarily because their medical records frequently fail to show a 'separately identifiable' E/M service beyond the standard care involved in a minor procedure. Cigna nearly rolled out a policy in 2023 that would have forced practices to submit full documentation for all claims using modifier 25 with E/M codes 99212-99215 alongside minor procedures. While the policy was put on hold after fierce pushback from the AAD and AMA, the writing is on the wall.
This near-miss was a warning shot. Payers are actively building the infrastructure to demand documentation upfront, effectively shifting the audit process from post-payment to pre-payment.
Crafting an Irrefutable Appeal
When a denial hits, your appeal needs to be a surgical strike, not a blind resubmission. A winning appeal letter makes an evidence-based argument that directly refutes the payer’s reason for denial. Your goal is to make it easier for the reviewer to overturn the denial than to uphold it. For more in-depth strategies, our guide on medical billing denial management offers a playbook for turning denials into dollars.
A solid appeal must include these three things:
- The De-Identified Medical Record: Attach the full note for the date of service. No shortcuts.
- A Narrative Summary: Don't make the reviewer hunt for the evidence. Write a brief paragraph that walks them through the note, pointing out the distinct chief complaint, HPI, and exam findings supporting the E/M service.
- Reference Payer and CMS Policies: Quote the payer’s own clinical policy on modifier 25 if you can find it. If not, cite the relevant section from the CMS Claims Processing Manual. This shows you’ve done your homework and documented according to their rules.
For instance, your appeal letter might state: "The attached record documents a significant, separately identifiable E/M service for the evaluation of a new, symptomatic nevus on the patient’s back (see HPI and Exam sections). This is distinct from the planned cryotherapy for actinic keratosis on the forearms. Per CMS guidelines, this justifies the use of modifier 25."
This direct, evidence-based approach is your best tool for protecting your revenue.
Turning Audits into Action: Remediation and KPIs
Finding modifier 25 compliance issues is one thing. Building a system to fix them is what actually protects your practice’s bottom line. A good remediation plan isn't about pointing fingers; it's about turning audit findings into practical provider education that creates a culture of continuous improvement. This is how you prove the ROI of your compliance work.
The goal is never punitive. It's about giving your providers clear, data-backed feedback that shows them exactly how their documentation habits impact the revenue cycle. For these sensitive conversations, skip the group meetings and email blasts. One-on-one sessions are the only way to go.
A Structured Process for Provider Education
Delivering feedback effectively requires both tact and hard data. When you sit down with a provider, come prepared with findings from their specific chart reviews. Focus on the patterns you're seeing, not just one-off mistakes. The best way to make the rules click is by using anonymized, side-by-side examples from your own audits.
Show them what works and what doesn't. For instance:
- The Problem Note: A chart where the evaluation of a new mole is just blended into the general exam note for a planned cryotherapy of actinic keratoses (CPT 17000). The two services are indistinguishable.
- The Compliant Note: A chart that uses a separate "New Lesion Evaluation" heading. It clearly documents a distinct HPI, exam, and MDM for the mole before moving on to the procedure portion of the note.
This kind of visual contrast makes the abstract rule of "significant, separately identifiable" tangible and easy to grasp. The conversation should be about how a few small changes to documentation habits can completely eliminate audit risk.
A successful remediation program is about coaching, not criticizing. Your objective is to make compliant documentation the path of least resistance for busy providers by giving them better tools, like refined EHR smart phrases, and a clear understanding of the 'why' behind the rules.
When you take this approach, the audit process shifts from a dreaded compliance task to a valuable tool for professional development. You empower providers to protect themselves and the practice from payer scrutiny.
Key Performance Indicators to Measure Success
You can't manage what you don't measure. Tracking a few specific KPIs is the only way to know if your remediation efforts are actually working and to show practice leadership that your compliance program is paying off. A focused dashboard gives you an at-a-glance view of your practice's modifier 25 health.
Start by tracking these critical metrics:
- Modifier 25 Denial Rate: Calculate this as a percentage of all claims submitted with modifier 25. You should be watching this monthly for each provider and for the practice as a whole. A steady downward trend is your number one sign of success.
- Internal Audit Pass Rate: What percentage of charts you review internally are meeting your compliance standards? If this number is climbing, it means your provider education is sticking.
- Financial Impact of Overturned Appeals: Track the exact dollar amount you recover from appealing wrongful modifier 25 denials. This metric is pure ROI for your appeals process.
- Average Days in A/R for Modifier 25 Claims: Are these specific claims getting stuck in accounts receivable longer than your other claims? A drop in this number means cleaner claims are getting paid faster.
These metrics tell a powerful story. They can help you spot whether a specific payer is getting more aggressive with denials or if a particular provider needs a bit more coaching. For a deeper look, our guide on the top medical billing KPIs to track can help you build an even more robust dashboard. This data-driven approach takes the emotion and guesswork out of the equation, letting you make smart business decisions that strengthen your revenue cycle.
What is the single biggest mistake in modifier 25 documentation?
The most common and costly mistake is "note bloat" from cloning previous encounter notes. When the documentation for the E/M service isn't clearly distinct from the procedure note, auditors will assume the work was incidental and not separately billable. Your note needs to tell two separate stories: one for the problem-focused E/M visit and one for the procedure. For example, if a patient comes in for a wart destruction (17110) but also asks you to evaluate a new, suspicious lesion, the HPI, exam, and MDM for that lesion evaluation must be documented as a completely distinct service from the wart treatment.
Can I use modifier 25 for a new patient visit?
Yes, you can absolutely use modifier 25 on a new patient E/M code (99202-99205) if you also perform a minor procedure on the same day. The key, as always, is that the E/M service must be significant and separately identifiable. In fact, this is often easier to justify with new patients, since the comprehensive evaluation is inherently separate from a quick decision to perform a minor procedure. Just make sure the documentation robustly supports the medical necessity for a full new patient workup in addition to the procedure itself.
How do I fight a modifier 25 denial for 'bundling'?
To fight a bundling denial, your appeal has to pinpoint exactly what made the E/M service separate and significant. Don't just resubmit the claim. You need to write a detailed appeal letter that includes the de-identified medical record and literally highlights or calls out the specific parts of the note (HPI, ROS, Exam, MDM) that correspond to the E/M service. If you can find the payer's own clinical policy on modifier 25, reference it directly, along with CMS guidelines. Clearly state: "The E/M service was for the evaluation of [Problem A], which was a separate clinical concern from the pre-operative work for the procedure addressing [Problem B]." This clear, concise narrative is your strongest weapon for overturning these denials. If you need expert backup for these complex denials, our specialized dermatology billing services are built to manage exactly this.